Hip Hip Hooray! Part I
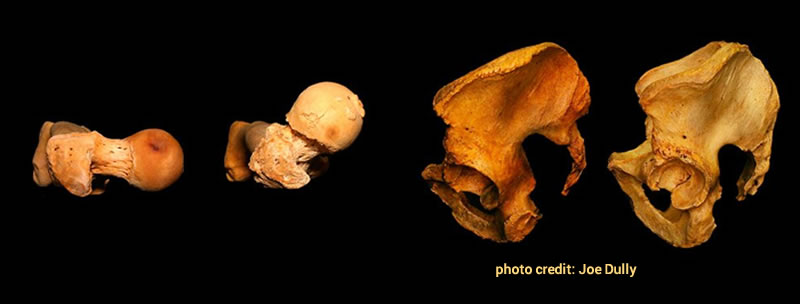
Last week I shared this article on Facebook, thanks Asia Nelson for sharing it with me. The interest it generated was encouraging. The article was written by a personal trainer questioning how people do squats. The images are from Paul Grilley’s web site. I have been referring to these images in my teacher training programs for years. The images are of two femurs and two pelvises from two different bodies. They depict how our bones vary in shape and proportion.
Typically squats are not part of most yoga regimes, but that is changing, thanks to the cross pollination that is taking place between fitness experts and yogis. Utkatasana (sometimes referred to as “chair pose”) is the pose that most resembles a squat. It’s taught with feet together and knees together. Some people can get quite low in the pose; others are stuck and can’t go any lower. There are many variations, and teachers who have a certain natural predisposition in their own bodies will tend to teach either a lower version where the knees are bent a lot or a higher version. If the low version is being taught there will be students in the room who, because of the shape of their bones, cannot go lower. Are those students being supported or are they being made to feel inadequate because they can’t go as deep? Does this approach encourage those students to try harder? I would answer ‘yes’ most of time. They try harder because they don’t think they’re getting enough out of the pose, so they push themselves into going lower with feet and knees together. Allowing those students to widen their stance and even turn out their feet would accommodate the shape of their bones. Because it does not match the picture of Utkatasana, it’s not often given as a variation.

The shape of our bones comes into play again when stepping forward into lunges or warrior poses. Allowing for a wider stance from right to left (as opposed to front to back) and allowing for a slight turnout in the front foot and knee to accommodate the natural turn out in some hip sockets could reduce the amount of friction in the hip joint. Why is this important?

There has been a tremendous amount of research done in the past decade on a condition called hip impingement. It is a condition where the head of the femur and the hip socket rub against one another. This causes friction of the cartilage (called the labrum) resulting in a tear. Risk factors include pre-existing structural abnormalities (i.e. people born with hip dysplasia) and overuse leading to repetitive strain and friction.
The symptoms include (taken from the Stanford Hospital web site)
- Pain or aching (usually located at the inner hip, or groin area), usually after walking, or prolonged sitting (such as in a car)
- A locking, clicking or “catching” sensation within the joint
- Pain sitting for long periods of time, like in a car
- Difficulty putting on your socks and/or shoes
- Difficulty walking up hill
- Low back pain
- Pain at the SI (sacroiliac joint on back of pelvis), the buttock, or greater trochanter (side of hip)
- It is often confused with other sources of pain, such as hip flexor tendinitis, pain from the back (disc or spine), testicular pain, sports hernia.
Sound familiar? I have known many yoga students and teachers who have complained of these symptoms and continued to do their practice, often assuming that they need to stretch more and go deeper into their poses to ‘work it out’.
This condition is becoming more common among middle-aged women who do a lot of yoga. The other day I ran into an ‘old regular’ from dwd, a guy who started to develop hip pain in certain standing postures. An MRI confirmed that he had hip impingement. His doctor told him to modify his practice and try to heal the condition or prepare for surgery that may lead to premature arthritis. It’ll be hard for a person who’s dedicated so many years trying to go deeper into their yoga practice only to realize that the very practice that healed him in so many ways also has the capacity to injure.
Here is what the Stanford Medical Hospital web site has to say:
‘Non-operative management of FAI can be attempted. However, it involves a change in lifestyle from active to less active and a commitment to maintaining hip strength. A good physical therapy program focusing on hip strengthening instead of stretching may be beneficial. Stretching associated with yoga and sometimes physical therapy may make the symptoms worse. Activity modification should involve avoiding activities that take the hip through extreme or full ranges of motion. Anti-inflammatory medications can also be attempted.’
Avoid taking the hip through extreme or full range of motion, what does mean?
Thanks for reading, questioning and the continued dialogue.
If you have questions about your practice come see me during those times.
Namaste,